Dante Luiz Escuissato 1, Flávia Sprenger 2, João Mário Clementin de Andrade 3
Abstracto
We present a case of a 62-year-old hypertensive and diabetic female that presented with severe pneumonia due to SARS-COV2 and required mechanical ventilation. Six days after intensive care unit admission she underwent computerized tomography due to clinical suspicion of bacterial secondary infection, which was confirmed by tomographic signs. This case is an important example of a classic and well indicated imaging exam in a case of COVID-19.Dados do caso
Feminino 62 anos
Palavras chaves
Pneumonia, Pneumonia Viral, Pneumonia Bacteriana
Histórico Clínico
A 62-year-old hypertensive and diabetic female patient presented to the emergency room with recent installation of fever and cough. After initial evaluation, she was admitted in the intensive care unit and required mechanical ventilation due to respiratory failure. COVID-19 diagnosis was made through PCR testing.
Achados Radiológicos
Chest radiograph was performed in the intensive care unit, revealing bilateral, predominantly peripheral and lower lung zone airspace opacities. Six days later patient underwent chest computerized tomography (CT) due to clinical suspicion of secondary bacterial infection. The chest- CT showed bilateral ground glass opacities with a predominant peripheral and lower lung zone distribution, probably related to COVID-19 and minimal bilateral effusion, bronchial impaction and collapse of the lower left lung, that can be with clinical hypothesis.
Discussão
The coronavirus disease 2019 (COVID-19) is a currently pandemic viral infection that may cause severe acute respiratory syndrome. Morbimortality is particularly higher amongst the elderly and patients with chronic diseases. Diagnosis is made through PCR detection of SARS-CoV2 [1]. Though most recommendations discourage the use of chest-CT as a screening tool, the number of patients undergoing imaging is increasing. Therefore, it is fundamental to radiologists recognise promptly signs that may suggest COVID-19[1]. Main findings include ground glass opacities with or without foci of consolidations with a predominant peripheral and posterior distribution, reverse halo sign and others organizing pneumonia features, diffuse opacities and areas with crazy paving pattern. Tree-in-bud centrilobular nodules, cavitation, isolated consolidation and septal thickening are considered atypical manifestations. Lymphadenopathy and pleural effusion are also not expected. Positive findings are more prevalent between six and thirteen days after initial symptoms [1]. Posterior and peripheral distributed ground glass opacities are the tomographic face of COVID-19. Computerized tomography is more sensitive than conventional radiographs and imaging can be negative, especially on the beginning of the symptoms [1]. Patient underwent CT due to recent leukocytosis, to search for signs of bacterial superinfection. On this clinical context, the finding of hypodense content on bronchi can relate to secondary infection. Antibiotic therapy was instituted, and the patient showed clinical improvement. Despite divergence and uncertainty in the literature, image methods have not been performed in most inpatients with COVID-19. Chest radiographs are useful and preferable in some clinical scenarios. Chest-CT is resourceful in suspicion of complications and differential diagnosis. Prognosis cannot be officially stated according to CT findings [2]. As radiologist, it is our responsibility to actively search for typical and atypical signs of viral pneumonia and its differential diagnosis.
Lista de Diferenciais
Diagnóstico
Aprendizado
We learned from this case to be alert to signs of COVID-19 but also signs of complications, in this case, secondary bacterial infection.
Referências
Imagens
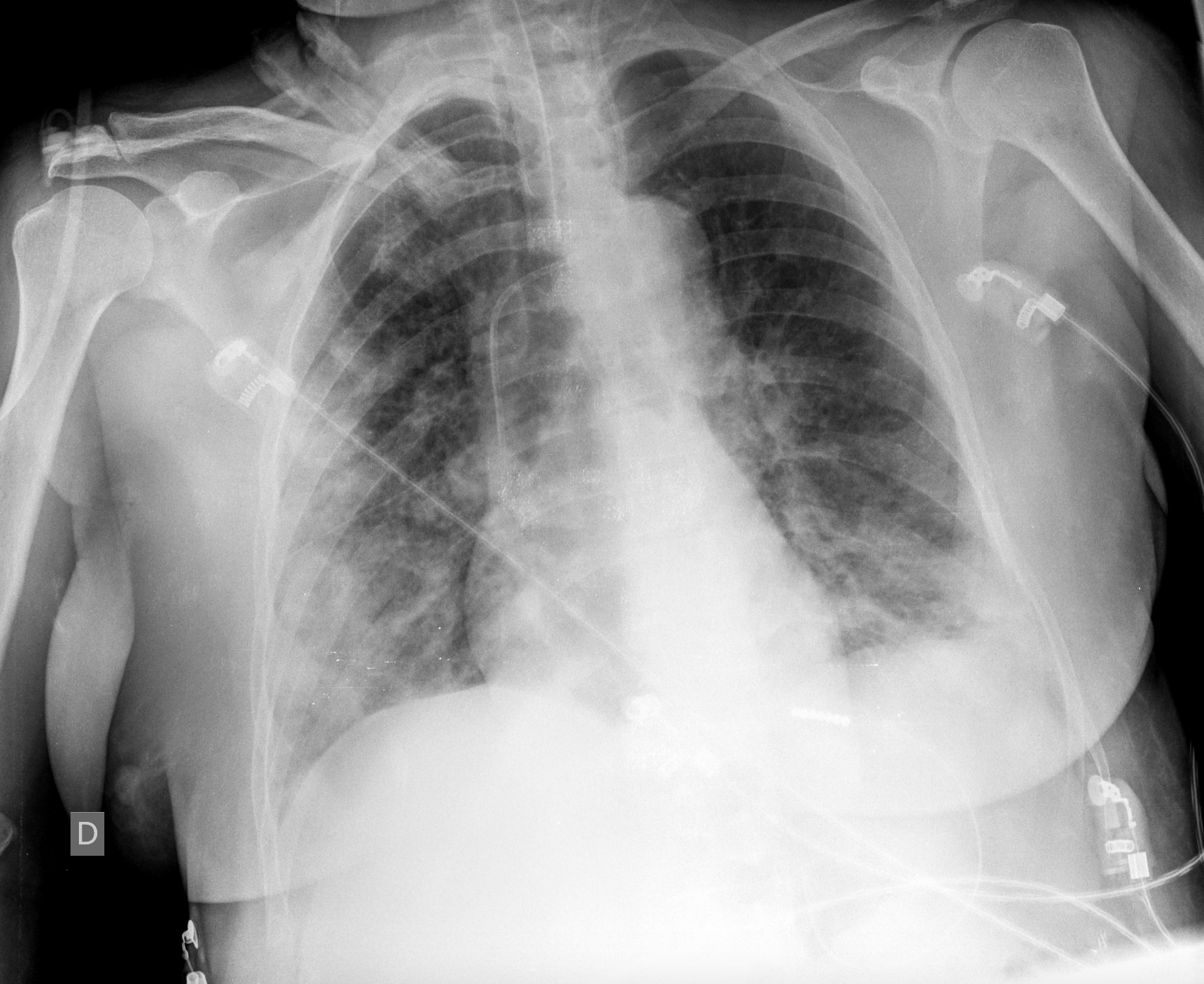
Figure 1: Chest radiograph performed at the admission in the intensive care unit. Notice multiple and bilateral foci of alveolar opacities, more evident in the lower right lung.
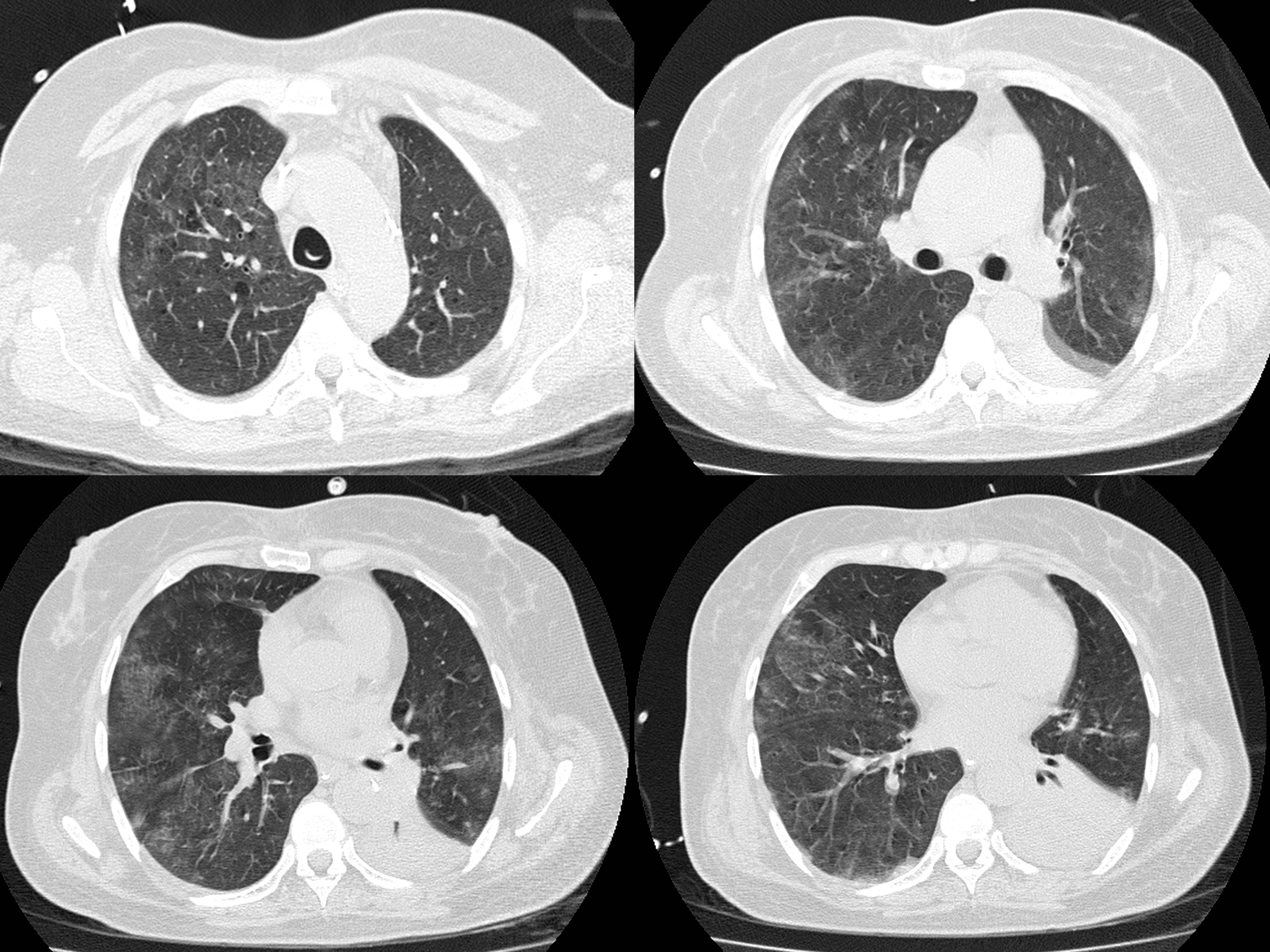
Figure 2: Axial images of CT performed six days later after intensive care unit admission. Multiple and bilateral ground glass opacities, with a predominant peripheral and basal distribution.
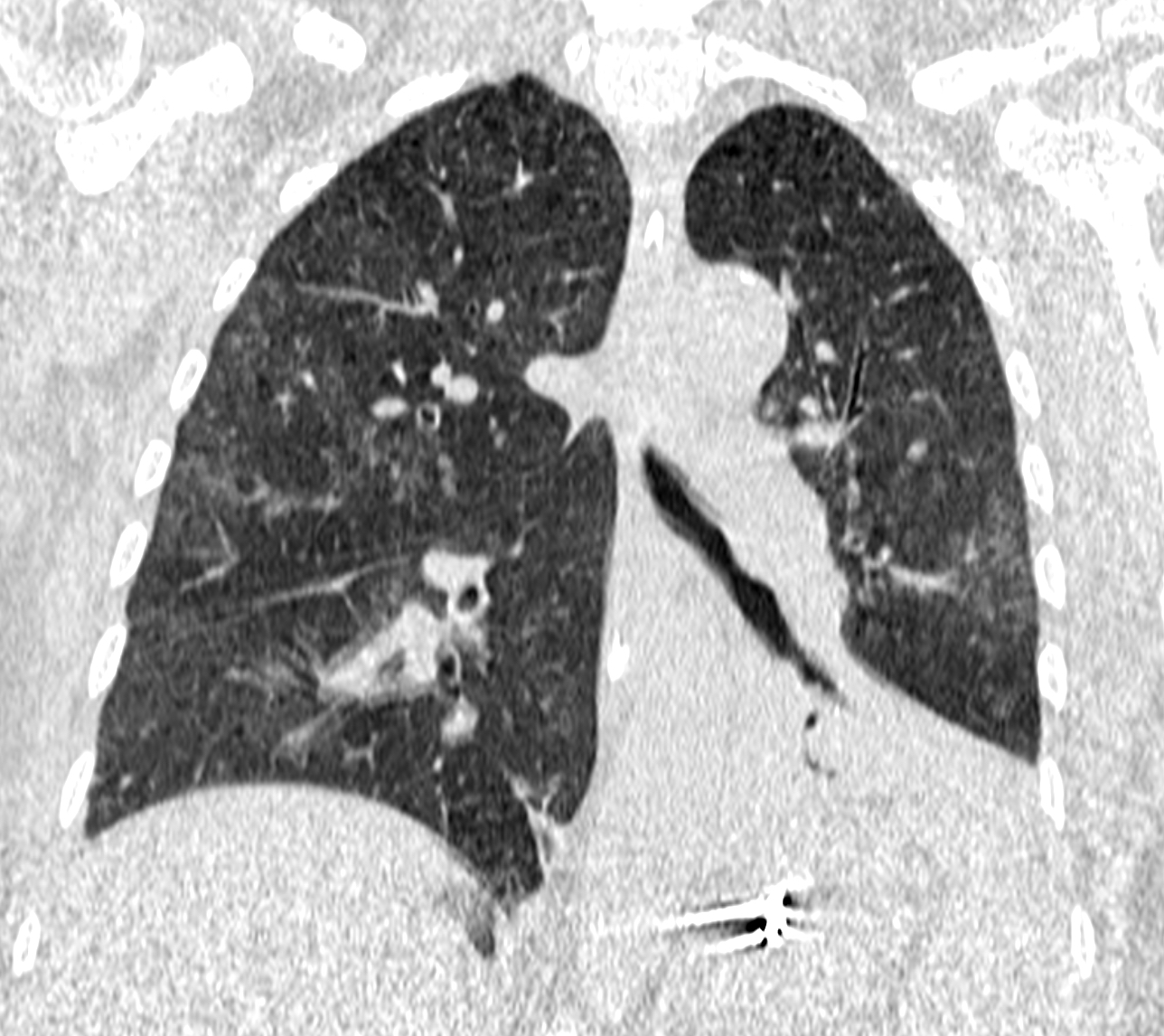
Figure 3: Coronal image of CT showing the predominant peripheral distribution of the ground glass opacities.
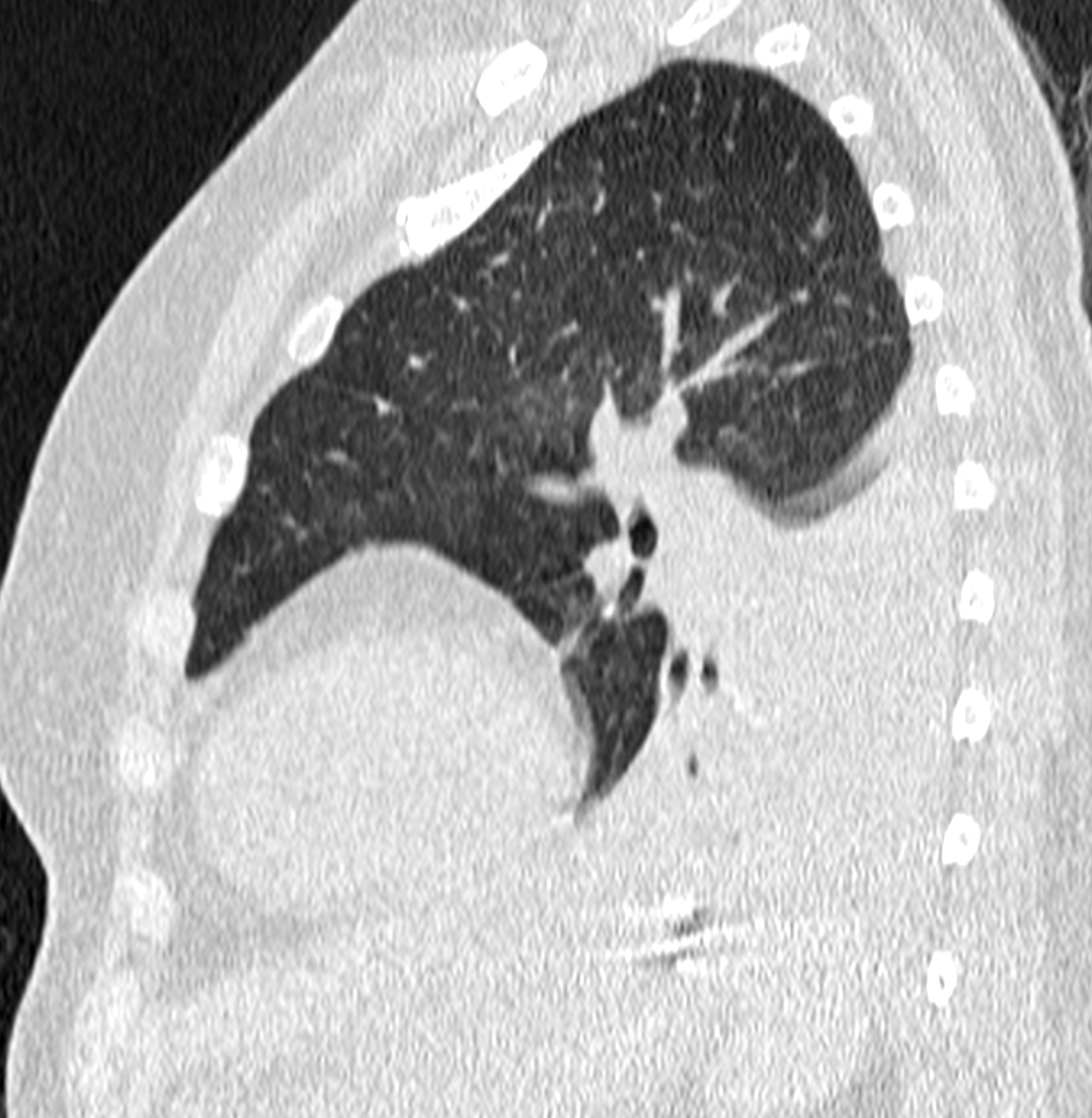
Figure 4: Partial collapse of the lower left lobe on sagittal CT image.
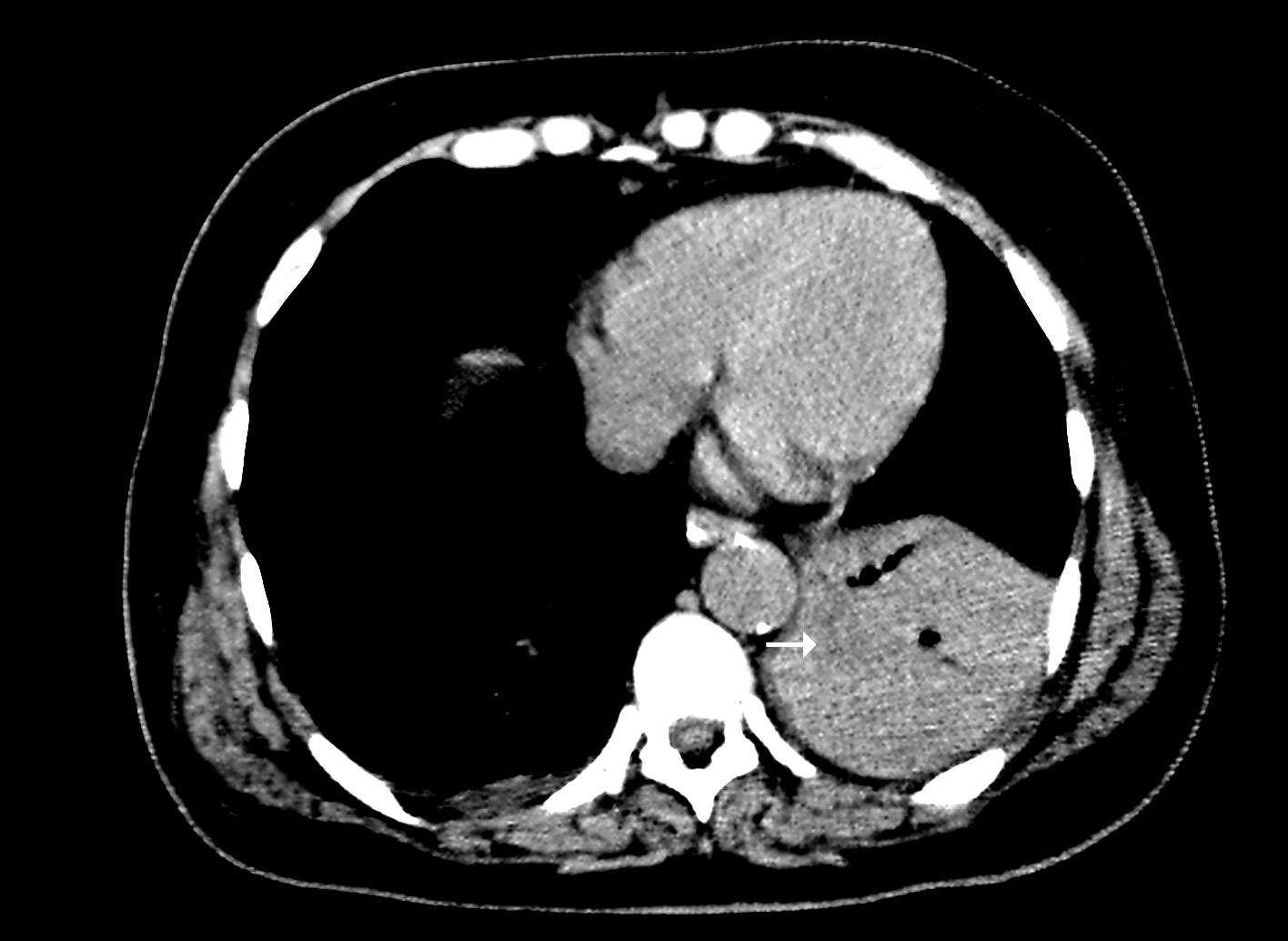
Figure 5: Notice the hypodense bronchi content on the collapsed parenchyma of the lower left lobe (arrow).
Vídeos
Artículo recibido en martes, 21 de abril de 2020
Artículo aceptado el lunes, 4 de mayo de 2020
 Todos los artículos científicos publicados en brad.org.br están bajo una licencia Creative Commons.
Todos los artículos científicos publicados en brad.org.br están bajo una licencia Creative Commons.